- Module 3
CBL 15:
______________________________________________________________________________
CBL 15 SENARIO: A 3-year-old boy (height 85 cm, -3 standard deviations (SD); weight 13 kg, approximately 10th percentile) presents with short stature. Review of the past history and growth chart demonstrates normal birth weight and birth length, but a progressive fall off in height velocity relative to age matched normal ranges starting at 6 months of age. physical examination demonstrates short stature and mild generalized obesity. Genital examination reveals descended but small testes and a phallic length of -2 SD. Laboratory evaluation demonstrates growth hormone (GH) deficiency and a delayed bone age of 18 months. The patient is started on replacement with recombinant human GH at a dose of 40 mcg/kg/d subcutaneously. After 1 year of treatment, his height velocity has increased from 5cm /year to 11 cm/ year. Learning outcomes: How does GH stimulate growth in children? What other hormone deficiencies are suggested by the patient’s physical examination?
What other hormone supplementation is this patient likely to require?
What are the side effects of hypothalamic and pituitary hormones?
- Module 2
CBL 14:
______________________________________________________________________________
CBL 14 SENARIO: A 59-year-old woman presents to an urgent care clinic with a 4-day history of frequent and painful urination. She has had fevers, chills, and flank pain for the past 2 days. Her physician advised her to come immediately to the clinic for evaluation. In the clinic she is febrile (38.5°C [101.3°F]) but otherwise stable and states she is not experiencing any nausea or vomiting. Her urine dipstick test is positive for leukocyte esterase. Urinalysis and urine culture are ordered. Her past medical history is significant for three urinary tract infections in the past year. Each episode was uncomplicated, treated with trimethoprim-sulfamethoxazole, and promptly resolved. She also has osteoporosis for which she takes a daily calcium supplement. The decision is made to treat her with oral antibiotics for a complicated urinary tract infection with close follow-up. Given her history, what would be a reasonable empiric antibiotic choice? Depending on the antibiotic choice are there potential drug interactions? Learning outcomes: Discuss the mechanism of action of sulphonamides Explain the spectrum of activity of sulphonamides
Discuss the uses and adverse effects of sulphonamides
CBL 13:
______________________________________________________________________________
CBL 13 SENARIO: A 45-year-old man with no medical history was admitted to the intensive care unit (ICU) 10 days ago after suffering third-degree burns over 40% of his body. He had been relatively stable until the last 24 hours. Now he is febrile (39.5°C [l 03.1°F]), and his white blood cell count has risen from 8,500 to 20,000/mm3. He has also had an episode of hypotension (86/50 mm Hg) that responded to a fluid bolus. Blood cultures were obtained at the time of his fever and results are pending. The ICU attending physician is concerned about sepsis and decides to treat with empiric combination therapy directed against Pseudomonas. The combination therapy includes tobramycin. The patient weighs 70 kg (154 lb) and has an estimated creatinine clearance of 90 mL/min. How should tobramycin be dosed using once-daily and conventional dosing strategies? How should each regimen be monitored for efficacy and toxicity? Learning outcomes: Discuss the mechanism of action of aminoglycoside. What are the adverse effects of aminoglycosides?
What are the precautions and dosing requirements for the renal patients?
CBL 12:
______________________________________________________________________________
CBL 12 SENARIO: A 55-year-old man is brought to the local hospital emergency department by ambulance. His wife reports that he had been in his normal state of health until 3 days ago when he developed a fever and a productive cough. During the last 24 hours he has complained of a headache and is increasingly confused. His wife reports that his medical history is significant only for hypertension, for which he takes hydrochlorothiazide and lisinopril, and that he is allergic to amoxicillin. She says that he developed a rash many years ago when prescribed amoxicillin for bronchitis. In the emergency department, the man is febrile (38.7°C [101.7°F]), hypotensive (90/54 mm Hg), tachypneic (36/min), and tachycardic (110/min). He has no signs of meningismus, but is oriented only to person. A stat chest x-ray shows a left lower lung consolidation consistent with pneumonia. The plan is to start empiric antibiotics and perform a lumbar puncture to rule out bacterial meningitis. What antibiotic regimen should be started to treat both pneumonia and meningitis? Does the history of amoxicillin rash affect the antibiotic choice? Why or why not? Learning outcomes: Discuss the classification of cell wall inhibitors Discuss the spectrum of cell wall synthesis inhibitors
Mechanism of action and resistance of cell wall synthesis
The causative bacteria and pharmacotherapy of pneumonia and meningitis
CBL 11:
______________________________________________________________________________
CBL 11 SENARIO: A 60-year-old man with a history of moderate chronic obstructive pulmonary disease presents in the emergency department with a broken hip suffered in an automobile accident. He complains of severe pain. What is the most appropriate immediate treatment for his pain? Are any special precautions needed? Learning outcomes: 1. Classify the opioids 2. Discuss the mechanism of action of opioids
3. What are the adverse effects of opioids specifically focusing on respiratory system?
4. Discus the physical dependence and tolerance phenomenon
CBL 10:
______________________________________________________________________________
CBL 10 SENARIO: A 48-year-old man presents with complaints of bilateral morning stiffness in his wrists and knees and pain in these joints on exercise. On physical examination, the joints are slightly swollen. The rest of the examination is unremarkable. His laboratory findings are also negative except for slight anemia, elevated erythrocyte sedimentation rate and positive rheumatoid factor. With the diagnosis of rheumatoid arthritis, he is started on a regimen of naproxen, 220 mg twice daily. After 1 week, the dosage is increased to 440 mg twice daily. His symptoms are reduced at this dosage, but he complains of significant heartburn that is not controlled by antacids. He is then switched to celecoxib, 200 mg twice daily, and on this regimen his joint symptoms and heartburn resolve. Two years Later, he returns with increased joint symptoms. His hands, wrists, elbows, feet, and knees are all now involved and appear swollen, warm, and tender. What therapeutic options should be considered at this time? What are the possible complications? Learning outcomes: 1. What are the side effects of NSAIDs 2. What are the therapeutic strategies of inflammatory diseases
3. Describe the role of COX-1 and COX-2
4. Considerations while Choice of NSAIDs
5. What is the treatment of R.A complication
6. Classify the NSAIDs
CBL 09: Epilepsy drugs
______________________________________________________________________________
CBL 09 SENARIO: A 23-year-old woman presents to the office for consultation regarding her antiseizure medications. Seven years ago, this otherwise healthy young woman had a generalized tonic clonic seizure (GTCS) at home. She was rushed to the emergency department, at which time she was alert but complained of headache. A consulting neurologist placed her on levetiracetam, 500 mg bid. Four days later, EEG showed rare right temporal sharp waves. MRI was normal. One year after this episode, a repeat EEG was unchanged, and levetiracetam was gradually increased to I000 mg bid. The patient had no significant adverse effects from this dosage. At age 21, she had a second GTCS while in college; further discussion with her roommate at that time revealed a history of two recent episodes of 1-2 minutes of altered consciousness with lip smacking (complex partial seizures). A repeat EEG showed occasional right temporal spikes. Lamotrigine was gradually added to the regimen to a dosage of 200 mg bid. Since then, the patient has been seizure-free for almost 2 years but now comes to the office for a medication review. Gradual discontinuation of levetiracetam is planned if the patient continues to do well for another year, although risk of recurrent seizures is always present when medications are withdrawn. Learning outcomes: What could be the outcomes of the Levetiracetam withdraw1? Explain the mechanism of seizures/epilepsy
Explain the mechanism of action of drugs used in the treatment of epilepsy
What are the adverse effects of anti-seizure drugs?
CBL 08: Anesthetics
______________________________________________________________________________
CBL 08 SENARIO: An elderly man with type 2 diabetes mellitus and ischemic pain in the lower extremity is scheduled for femoral-to-popliteal bypass surgery. He has a history of hypertension and coronary artery disease with symptoms of stable angina and can walk only half a block before pain in his legs force him to stop. He has a 50 pack-year smoking history but stopped 2 years ago. His medications include atenolol, atorvastatin, and hydrochlorothiazide. The nurse in the preoperative holding area obtains the following vital signs: Temperature 36.8 ˚C (98.2 ˚F), blood pressure 168/100 mm Hg, heart rate 78 bpm, oxygen saturation by pulse oximeter 96% while breathing room air, pain 5/10 in the right lower leg.
Learning outcomes: What anesthetic agents will you choose and why? Does the choice of anesthetic make a different?
Discuss the mechanism of action of anesthetics
CBL 07: Anxiolytics / Hypnotic drugs
______________________________________________________________________________
CBL 07 SENARIO: At her annual physical examination, a 53-year old middle school teacher complains that she has been experiencing difficulty falling asleep and after falling asleep awakens several times during night. These episodes occur almost nighty and are having a negative impact on her teaching functions. She has tired varies over the counter sleep remedies, but they were of little help and she experienced hangover effects the next day. Her general health is good, she is not overweight, and she takes no prescription drugs. She drinks one cup of decaffeinated coffee in the morning however, she drinks one cup of decaffeinated coffee in the morning however, she drinks as many as six cans per day of diet cola. She drinks a glass of wine with her evening meal but does not like stronger spirits. Learning outcomes: What other aspects of this patient’s history would you like to know? What therapeutic measure are appropriate for this patient?
What drug, or drugs (if any), would you prescribe?
Discuss the mechanism of anxiolytics/hypnotic’s drugs?
- Module 1
CBL No: 06 SENARIO: A 49-years old man with a history of congenital heart disease has a successful cardiac transplant 6 months ago. He is now admitted to the hospital in severe agitation. He is found to have a blood pressure of 170/110 mm hg, heart rate 130, respiration 35, sweating and cutaneous vasoconstriction. He admits to it self-injecting methamphetamine 4 hours previously. How does methamphetamine increase blood pressure? Normally, heart rate would be greatly reduced with this degree of drug-induced hypertension. Why is this patient’s heart rate elevated Learning outcomes: Mechanism of action of Methamphetamine. Adverse effect (short + long term).
Clinical use of methamphetamines.
Effect of dopamine, epinephrine and nor- epinephrine on heart.
CBL No: 05 SENARIO: Mrs Jameel, 45 years of age, is a housewife. Since last few months she was feeling fatigue of shoulder muscle while combing her hair. She had to perform some unusual physical work when her family was to move into a new residence and all the luggage and house hold was to be packed for shifting. She felt extremely weak during the activity and was compelled to take rest at short intervals. Learning outcomes: What is Myasthenia gravis? Explain etiology and patho-physiology of the disease.
Analyze the Approaches to pharmacotherapy of myasthenia gravis.
Enlist the classification of anticholinesterase drugs.
Explain the mechanism of action of anticholinesterases.
Discuss the adverse effects of anticholinesterases and their control
How to distinguish between cholinergic crisis and myasthenia crisis.
Discuss the uses of anticholinesterases.
Identify the drugs that may precipitate myasthenia gravis.
Learning resources: Basic and clinical Pharmacology by Bertram G Katzung 13th Edition The Pharmacological Basis of Therapeutics by Goodman & Gilman 12th Edition
Current Medical Diagnosis and treatment- 2015
CBL 04 A 68-year-old man presents with a complaint of lightheadedness on standing that is worse after meal and in hot environment. Symptoms started about 4 year ago and have slowly progressed to the point that he is disabled. He is fainted several times, but always recovers consciousness almost as soon as he falls. Review of symptoms reveals slight worsening of constipation, urinary retention out of proportion prostate size, and decrease sweating. He is otherwise healthy with no history of hypertension diabetes, orparkinson’s disease. Because of his urinary retention, he was placed on the α1 antagonist tamsulosin but he could not tolerate it because of worsening of orthostatic hypotension. Physical examination revealed a blood pressure of 167/84 mm Hg supine and 106/55 mm Hg standing. There was an inadequate compensatory increase in heart rate (from 84 to 88 bpm), considering the degree of orthostatic hypotension. Physical examination is otherwise unremarkable with no evidence of peripheral neuropathy or parkinsonian features. Lab examinations are negative expect for plasma norepinephrine, which is low at 98 pg/ml (normal is 250-400 pg/ml for his age). A diagnosis of pure autonomic failure is made, based on the clinical picture & the absence of drug that could induce orthostatic hypotension and disease commonly associated with autonomic neuropathy (e.g, diabetes, parkinso’s disease). What precaution should this patient observe in using sympathomimetic drugs? Can such drugs be used in his treatment? Learning outcomes: What are the physiological effect of catecholomines on body. Classification of sympathomimetic drugs.
Sites of action & effects on different system.
Adverse effects of sympathomimetic drugs.
Clinical uses of sympathomimetic drug.
CBL 03 A 16-year-old female come to ER, four hours after ingestion of insecticides (organophosphate). ON EXAMINATION 1. Altered consciousness, pupil constricted, Frothing from mouth 2. On auscultation; Tachypnoea and crepitation VITALS: Pulse 60/min, Respiratory 30/min, B.P 90/60 mmHg The intern on duty started I.V fluids and gave antidote pralidoxime but the condition of the patient further deteriorated, until physician came and started atropine I/v in small doses after fix intervals. The intern was curios & asked clinical pharmacologist about the role of antidote. He explained the role of antidote in this case by a graph.

TASK: Interpret the graph and discuss the role of antagonist drugs and their types. Learning outcomes: Interpret the concept of agonist & antagonists
Explain the Types of antagonism
Understand the graph and ability to draw graph from given information.
Explain the mechanism of action of organophosphate.
Correlate the signs & symptoms of organophosphate poisoning
Explain the Role of atropine & oximes in treatment
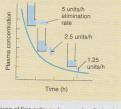
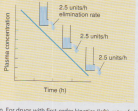
CBL 02 A 17- year old, patient known case of asthma was prescribed the grad tablet (theophylline) by the physician 600mg/day in two divided doses. He took four tablets of 300mg in 24 hours and came in ER with complain of nausea, headache, G.I distress, tachycardia and his ECG indicated arrhythmia. He was anxious and asked his physician that he never developed toxic effect whenever he took analgesics in high doses. INVESTIGATION: Blood theophylline level………22mg/l Serum keratinize 1.2mg/dl Serum urea 18mg/dl Liver function test (L.F.T) were normal TASK Discus the development of toxic effect and related Pharmacologic parameters. Learning outcomes: Concept of safety & efficacy Therapeutic index Concept of toxicity Factors effecting dose and toxicity Concept of correlation of half-life e- dose adjustment CBL 01 SENARIO: A group of research student conducted a preclinical trial of two different drugs to establish safely and efficacy and to study Pharmacokinetic and Pharmacodynamic profile. Two different Rabbits of same size were taken and injected with either one of the drug labeled as A & B. They collected serial blood sample from each rabbit after fix intervals and measured drugs level and then plotted a graph to study the plasma concentration rate of elimination of drugs from the body.
TASK Interpret the graph and discuss and compare the Pharmacokinetic profile of the drugs Learning outcomes: Explain the pharmacokinetics and pharmacodynamics Discuss the concept of half life and elimination of drug Explain the concept of zero order & first order kinetic. Interpret the concept of dose response curve Explain volume of distribution, clearance & bioavailability